3 Best Nursing Care Plans for Pressure Ulcers Based on Diagnosis
This article discusses Nursing Care Plans for Pressure Ulcers plus its causes, symptoms, preventions, treatments, and interventions.
Permalink: https://customnursingassignments.com/nursing-care-plans-for-pressure-ulcers
customnursingassignments.com has the top and most qualified writers to help with any of your assignments. All you need to do is place an order with us.(Nursing Care Plans for Pressure Ulcers)
Disclaimer: The information presented in this article is not medical advice; it is meant to act as a quick guide to nursing students for learning purposes only and should not be applied without an approved physician’s consent. Please consult a registered doctor in case you’re looking for medical advice.
Introduction
Pressure ulcers (also known as pressure sores or bedsores) are injuries to the skin and underlying tissue, primarily caused by prolonged pressure on the skin. Ulcers are more common on bony prominences with less cushioning between bone and skin (such as elbows, coccyx, and heels). They can also manifest themselves in other parts of the body. They can happen to anyone but usually affect people confined.
These breaks may not heal on their own because bacteria on the person’s skin or clothing colonize deep into the wet wound bed, causing it to become infected. The assessment and diagnosis of pressure ulcers, as well as risk factors, consequences, and therapies, are discussed in this blog post.
Pressure ulcers can develop over hours or days. Most sores heal with treatment, but some never heal completely. You can take steps to help prevent bedsores and help them heal.
Pressure Ulcers
A pressure ulcer, also known as bedsore or decubitus ulcer, is a localized skin injury caused by tissue compression between bony prominences and hard surfaces like a mattress. Pressure, in combination with friction, shearing forces, and moisture, causes them. Small blood arteries are compressed by the pressure, resulting in poor tissue perfusion. Reduced blood flow induces tissue hypoxia, which results in cellular death.
Common sites of pressure ulcers
Pressure ulcers on the skin across the following locations are common in wheelchair users:
- Buttocks or tailbone
- Spine and shoulder blades
- Backs of arms and legs where they rest against the chair
- Backs of arms and legs where they rest against the chair
- Pressure ulcers can occur in people who have to stay in bed for long periods of time.
- The back or sides of the head.
- The shoulder blades.
- The hip, lower back, or tailbone.
- The skin behind the knees, the heels, and the ankles.
Types of Pressure Ulcers
Bedsores, decubitus ulcers, and trochanteric bursitis are the most prevalent types of pressure ulcers. They don’t all cause deep tissue injury. They can be further divided into the following categories:
Dry ulcers
When scraped, the skin is dry and does not bleed. The tissue’s blood supply may be harmed or destroyed. The area feels firm to the touch.
Wet/Moist ulcers
A damp or moist feeling is common with this form of pressure ulcer. When the wounded region is scraped, the skin may bleed, and inflammation manifests itself as redness, swelling, and warmth.
Cold ulcers
When this sort of ulcer is touched, it does not cause pain or bleeding. Instead, due to a lack of blood flow, the tissue will be cold (also known as poor perfusion). It’s possible that your skin will appear pale and even frosty.
Sterile ulcers
An ulcer of this sort is red, swollen, and heated to the touch. The tissue’s blood supply has been cut off or diminished, but there are no microorganisms in the area.
Will Not Heal Pressure ulcers
This type of pressure sore has not responded to treatment and will not heal without surgical intervention.
Symptoms of pressure ulcers
Pressure ulcers can affect any part of the body that’s put under pressure. They’re most common on bony parts of the body, such as the heels, elbows, hips and base of the spine.
They often develop gradually but can sometimes form in a few hours.
Early symptoms
- Part of the skin becoming discoloured – people with pale skin tend to get red patches, while people with dark skin tend to get purple or blue patches.
- Discoloured patches not turning white when pressed
- A patch of skin that feels warm, spongy or hard
- Pain or itchiness in the affected area
Later symptoms
- An open wound or blister – a category two pressure ulcer
- A deep wound that reaches the deeper layers of the skin – a category three pressure ulcer
- A very deep wound that may reach the muscle and bone – a category four pressure ulcer
Risk factors of pressure ulcers
Suppose you have trouble moving and changing positions when seated or in bed; you’re more likely to acquire bedsores. The following are some of the risk factors:
Immobility. This could be due to a variety of factors, including poor health, spinal cord injury, and others.
Incontinence. When skin is exposed to urine and stool for an extended period of time, it becomes more susceptible.
Lack of sensory perception. Sensation loss can occur as a result of spinal cord injury, neurological illnesses, and other conditions. Lack of awareness of warning indicators and the need to shift positions can stem from an inability to feel pain or discomfort.
Medical conditions affecting blood flow. Diabetes and vascular illness, both of which can impair blood flow, might increase the risk of tissue damage such as bedsores.
Deficiency in nutrients and hydration. To maintain healthy skin and avoid tissue breakdown, people require enough water, calories, protein, vitamins, and minerals in their daily diets.
Stages of Pressure Ulcers
The stages are determined by the depth of the sores, which has an impact on how they are treated.
If caught early, these sores are likely to heal in a few days with little fuss or pain. Without treatment, they can get worse.
When the sore shrinks and pink tissue appears along the sides, you’ll know they’re getting better.
The stages include:
Stage 1
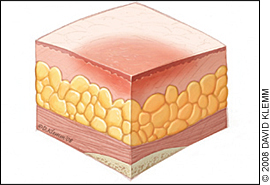
This is the mildest stage. These pressure sores only affect the upper layer of your skin.
Symptoms: Pain, burning, or itching are common symptoms. The spot may also feel different from the surrounding skin: firmer or softer, warmer or cooler.
You may notice a red area on your skin. If you have darker skin, the discoloured area may be harder to see. The spot doesn’t get lighter when you press on it, or even 10 to 30 minutes after you stop pressing. This means less blood is getting to the area.
What to do: The first and most important thing to do with any pressure sore is to stop the pressure. Change your position or use foam pads, pillows, or mattresses.
If you spend a lot of time in bed, try to move at least once every 2 hours. If you’re sitting, move every 15 minutes. You may need someone to help you.
Wash the sore with mild soap and water and dry it gently.
It may help to eat a diet high in protein, vitamins A and C, and the minerals iron and zinc. These are all good for your skin. Also, drink plenty of water.
Recovery time: A Stage 1 pressure sore may go away in as little as 2 or 3 days.
Stage 2
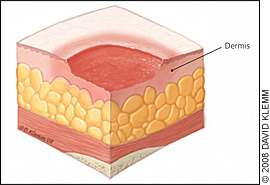
This happens when the sore digs deeper below the surface of your skin.
Symptoms: Your skin is broken, leaves an open wound, or looks like a pus-filled blister.
The area is swollen, warm, and/or red. The sore may ooze clear fluid or pus. And it’s painful.
What to do: Follow the same steps for Stage 1. You should also clean the wound with water or a salt-water solution and dry it gently. This may hurt, so ask your doctor if you should take a pain reliever 30 to 60 minutes before cleaning.
Keep the sore covered with a see-through dressing or moist gauze. If you see signs of an infection (such as pus, fever, or redness), tell your doctor.
Recovery time: A Stage 2 pressure sore should get better in 3 days to 3 weeks.
Stage 3
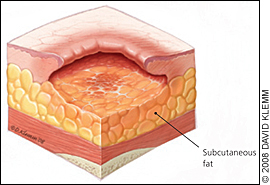
These sores have gone through the second layer of skin into the fat tissue.
Symptoms: The sore looks like a crater and may have a bad odour. It may show signs of infection: red edges, pus, odour, heat, and/or drainage. The tissue in or around the sore is black if it has died.
What to do: Stage 3 sores will need more care. Talk to your doctor. They may remove any dead tissue and prescribe antibiotics to fight infection. You may also be able to get a special bed or mattress through your insurance.
Recovery time: A Stage 3 pressure sore will take at least one month and up to 4 months to heal.
Stage 4
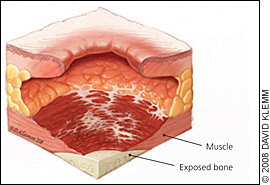
These sores are the most serious. Some may even affect your muscles and ligaments.
Symptoms: The sore is deep and big. The skin has turned black and shows signs of infection — red edges, pus, odour, heat, and/or drainage. You may be able to see tendons, muscles, and bones.
What to do: Tell your doctor right away. These wounds need immediate attention, and you may need surgery.
Recovery time: A Stage 4 pressure sore could take anywhere from 3 months or much longer, even years, to heal.
Causes of Pressure Ulcers
Pressure ulcers are caused by pressure against the skin that limits blood flow to the skin. Limited movement can make skin vulnerable to damage and lead to the development of pressure ulcers.
Three primary contributing factors for pressure ulcers are:
Pressure – Constant pressure on any part of your body can lessen the blood flow to tissues. Blood flow is essential for delivering oxygen and other nutrients to tissues. Without these essential nutrients, skin and nearby tissues are damaged and might eventually die. For people with limited mobility, this kind of pressure tends to happen in areas that aren’t well-padded with muscle or fat and that lie over a bone, such as the spine, tailbone, shoulder blades, hips, heels and elbows.
Friction – Friction occurs when the skin rubs against clothing or bedding. It can make fragile skin more vulnerable to injury, especially if the skin is also moist.
Shear – Shear occurs when two surfaces move in the opposite direction. For example, when a bed is elevated at the head, you can slide down in bed. As the tailbone moves down, the skin over the bone might stay in place — essentially pulling in the opposite direction.
Complications
The following are some of the life-threatening complications of pressure ulcers:
Cellulitis – Cellulitis is an infection of the skin and soft tissues that surround it. It might cause the affected area to become heated, red, and swollen. People with nerve damage frequently do not experience pain in the cellulitis-affected area.
Bone and joint infections – A pressure sore infection can spread to joints and bones. Infections in the joints (septic arthritis) can cause cartilage and tissue damage. Joint and limb function can be harmed by bone infections (osteomyelitis).
Cancer – Squamous cell carcinoma can arise from long-term, non-healing wounds (Marjolin’s ulcers).
Sepsis – A skin ulcer can cause sepsis in rare cases.
Preventions for pressure ulcers
It can be difficult to completely prevent pressure ulcers, but there are some things you or your care team can do to reduce the risk.
These include:
- Regularly changing your position – if you’re unable to change position yourself, a relative or carer will need to help you
- Checking your skin every day for early signs and symptoms of pressure ulcers – this will be done by your care team if you’re in a hospital or care home.
- Having a healthy, balanced diet that contains enough protein and a good variety of vitamins and minerals.
- Stopping smoking – smoking makes you more likely to get pressure ulcers because of the damage caused to blood circulation.
As you continue, customnursingassignments.com has the top and most qualified writers to help with any of your assignments. All you need to do is place an order with us. (Nursing Care Plans for Pressure Ulcers)

Nursing Diagnosis for Pressure Ulcers
Diagnosis involves;
- Physical examination to check for signs such as erythema and fluid seeping from the lesion.
- Impaired circulation—what could be the cause? Is it a vascular problem or a result of your position?
- To look for signs of infection, such as redness, swelling, discomfort, and a raised temperature.
- Lab tests to see if the patient has an infection or another ailment. Urine analysis, cultures, and blood counts are examples of these assays.
Nursing Care Plans for Pressure Ulcers
Pressure ulcers stage I through III can be managed with aggressive local wound treatment and proper nutritional support, while stage IV pressure ulcers usually require surgical intervention.
Measuring the contributing variables leading to a lack of tissue perfusion, assessing the extent of the injury, increasing medication compliance, and preventing additional harm is all part of nursing care for clients with pressure ulcers (bedsores).
Nursing Care Plan Based on Impaired Skin Integrity Diagnosis – Nursing Care Plans for Pressure Ulcers
Nursing Diagnosis: Impaired Skin Integrity
It may be related to:
- Chronic disease state.
- Extreme of ages.
- Imbalanced nutritional state.
- Impaired cognition.
- Impaired sensation.
- Immobility.
- Immunological deficit.
- Incontinence.
- Mechanical factors (friction, pressure, shear).
- Moisture.
- Poor circulation.
- Pronounced body prominence.
- Radiation.
Evidence of on Impaired Skin Integrity Diagnosis
- Destruction of skin layers.
- Disruption of skin surfaces.
- Drainage of pus.
- Invasion of body structures.
- Pressure ulcer stages:
- Deep tissue injury (new stage):
Purple or localized maroon area of intact skin or blood-filled blister resulting from pressure damage of underlying soft tissue.
- Stage I:
The epidermis is intact.
Non-branch able erythema of intact skin. Discolouration of the skin, warmth, edema, induration or hardness may also be used as indicators, particularly on individuals with darker skin.
- Stage II:
Partial-thickness skin loss involving epidermis, dermis, or both. The ulcer is superficial and presents clinically as an abrasion or blister.
- Stage III:
Full-thickness skin loss involving damage to or necrosis of subcutaneous tissue that may extend down to, but not through, underlying fascia.
Slough may be present; it may include undermining and tunnelling.
As you continue, customnursingassignments.com has the top and most qualified writers to help with any of your assignments. All you need to do is place an order with us. (Nursing Care Plans for Pressure Ulcers)

- Stage IV:
Extensive destruction, tissue necrosis or damage to muscle, bone or supporting structures, with or without full-thickness skin loss.
Undermining and tunnelling may develop.
- Unstageable:
Full-thickness tissue loss in which actual depth of ulcer is completely obstructed by slough or eschar in the wound bed.
Desired Outcomes
The client will get stage-appropriate wound care and has controlled risk factors for the prevention of additional ulcers.
The client will experience healing of pressure ulcers and experiences pressure reduction.
| Nursing Interventions | Rationale |
| Assess the specific risk factors for pressure ulcers: | Even clients with an existing pressure ulcer continue to be at risk for further injury. Nurses should consider all potential risk factors for pressure ulcers development. |
| Determine the client’s age and general condition of the skin. | Elderly clients have less elastic skin, less moisture, less padding and have thinning of the epidermis, making it more prone to skin impairment. |
| Assess the client’s nutritional status, including weight, weight loss, and serum albumin levels, if indicated. | A severe protein depletion has an albumin level of less than 2.5 g/dL. Clients with pressure ulcers lose large amounts of protein in wound exudates and may require 4000 kcal/day or more to remain anabolic. |
| Assess for a history of preexisting chronic diseases (e.g., diabetes mellitus, acquired immune deficiency syndrome, Guillain-barré syndrome, peripheral and/or cardiovascular disease). | Clients with chronic diseases typically exhibit multiple risk factors that predispose them to pressure ulceration. These include poor nutrition, poor hydration, incontinence, and immobility. |
| Assess the skin on admission and daily for an increasing number of risk factors. | The incidence of skin breakdown is directly related to the number of risk factors present. |
| Assess for a history of radiation therapy. | Irradiated skin becomes thin and brittle, may have less blood supply, and is at a higher risk for skin breakdown. |
| Assess the client’s awareness of the sensation of pressure. | Usually, people shift their weight off pressure areas every few minutes; this occurs more or less automatically, even during sleep. Clients with decreased sensation are unaware of unpleasant stimuli and do not shift weight, thereby exposing the skin to excessive pressure. |
| Assess for fecal and urinary incontinence. | The urea in urine turns into ammonia within minutes and is erosive to the skin. At the same time, the stool may contain enzymes that cause skin breakdown. Diapers and incontinence pads with plastic liners trap moisture and speed up breakdown. |
| Assess client’s ability to move (shift weight while sitting, turn over in bed, move from the bed to a chair). | Immobility is a huge risk factor for pressure ulcer development among adult hospitalized clients. |
| Assess for environmental moisture (excessive perspiration, high humidity, wound drainage). | Moisture may contribute to skin maceration. |
| Assess the amount of shear (pressure exerted laterally) and friction (rubbing) on the client’s skin. | Shearing forces are most commonly noted on the sacrum, scapulae, heels, and elbows from skin-sheet friction, from semi-Fowler’s position and repositioning, and from lift sheets. |
| Assess the surface that the clients spend a majority of time on (mattress for bedridden clients, cushion for clients in wheelchairs). | Clients who spend the majority of their time on one surface need a pressure reduction or pressure relief device to reduce the risk of skin breakdown. |
| Assess the skin over bony prominences (sacrum, trochanters, scapulae, elbows, heels, inner and outer malleolus, inner and outer knees, back of the head). | These areas are at the highest risk for breakdown resulting from tissue ischemia from compression against a hard surface. |
| Use an objective tool for pressure ulcer risk assessment: Braden scale. Norton scale. | The Braden scale is the most widely used risk assessment. It consists of six subscales, namely: activity, mobility, moisture, nutrition, sensory perception, and friction. Acute care: Assessment should be carried out on all patients on admission and every 24 to 48 hours or sooner if the patient’s condition changes. Long-term care: Assess on admission, weekly for four weeks, then quarterly and whenever the resident’s condition changes. |
| Assess the client’s level of pain, especially related to dressing change and procedures. | Prophylactic pain medication may be indicated. |
| Assess and stage the pressure ulcers. | Staging is essential because it determines the treatment plan. Staging should be assessed at each dressing stage. It reflects whether the epidermis, dermis, fat, muscle, bone, or joint is exposed. If the ulcer is covered with necrotic tissue (eschar), it cannot be accurately staged. Stage I ulcers are difficult to detect in darkly pigmented skin. The use of mirrors or a penlight may be helpful. |
| Determine the condition of the wound or wound bed. | |
| Presence of necrotic tissue. | Necrotic tissue is a tissue that is dead and eventually must be removed before healing can take place. Necrotic tissue exhibits a wide range of appearances: black, brown, leathery, hard, shiny, thin, tough, white. |
| Colour. | The colour of tissue is an indication of tissue viability and oxygenation. White, gray, or yellow eschar may be present in stage II and III ulcers. Eschar may be black in stage IV ulcers. |
| Odour. | An odour may arise from infection present in the wound; it may also arise from the necrotic tissue. Some local wound care products may create or intensify the odours and should be distinguished from wound or exudate odours. |
| Viability of bone, joints, or muscle. | In stage IV pressure ulcers, these may be apparent at the base of the ulcer. Wounds may demonstrate multiple stages or characteristics in a single wound. |
| Measure the size of the ulcer, and note the presence of undermining. | The ulcer dimensions include length, width, and depth. An ulcer begins in the deepest tissue layers before the skin breaks down. Hence the opening of the skin’s surface may not represent the true size of the ulcer. |
| Assess the condition of wound edges and surrounding tissue. | The surrounding tissue may be healthy or may have various degrees of impairment. Healthy tissue is necessary for the use of local wound care products requiring adhesion to the skin. The presence of healthy tissue demarcates the boundaries of the pressure ulcer. |
| Assess the wound exudate. | Exudate is a normal part of wound physiology and must be differentiated from pus which is an indication of infection. Exudate may contain serum, blood, and white blood cells and may appear clear, cloudy, or blood-tinged. The amount may vary from a few cubic centimetres, which are easily managed with dressings, to copious amounts not easily managed. Drainage is considered excessive when dressing changes are needed more often than every 6 hours. |
| Assess ulcer healing using a pressure ulcer scale for healing (PUSH) tool. | This tool provides standardization in the measurement of wound healing. It quantifies surface area, exudate, and the type of wound tissue. |
| Provide local wound care: | |
| Stage I: | |
| Apply a topical vasodilator (e.g., Proderm) | It increases skin circulation. |
| Apply a flexible hydrocolloid dressing (e.g., Duoderm) or a vapour-permeable membrane dressing (Tegaderm). | It prevents shear and friction. |
| Apply a vitamin-enriched emollient to the skin every shift. | It moisturizes the skin. |
| Stage II: | |
| Apply Alginates (Sorbsan, Kalginate, Kaltostat). | Alginate dressings are a type that is highly absorbent and so can absorb the fluid (exudate) that is produced by some ulcers. These are often used for ulcers with moderate-to-heavy exudate. |
| Apply hydrocolloids or a vapour-permeable membrane dressing. | Hydrocolloids are used to promote healing and wound debridement. They are not advised to use for heavy-exudate-producing wounds. |
| Apply gauze with sodium chloride solution. | This maintains a moist environment but requires multiple dressing changes. Dressings must be removed while still wet. Dressings absorb small amounts of drainage. |
| Apply Hydrogels (Carrasyn V, Aqua Skin). | Hydrogels provide moisture to dry, sloughy or necrotic wounds and assists autolytic debridement. It can be used on wounds with low exudate and is usually used for shallow ulcers without exudates. |
| Stage III and IV: | |
| Foams. | Different foams have different levels of absorbency. They are best used on granulating wounds. Foams lessen odour and repel bacteria and water. |
| Gauze with sodium chloride solution. | This maintains a moist environment but requires multiple dressing changes as described for stage II. |
| Wound fillers. | Wound fillers are used as a primary dressing and to pack wounds, maintain a moist environment. |
| Autolytic debridement. | Using a hydrocolloid or hydrogel, these create a moist wound interface that enhances the activity of endogenous proteolytic enzymes within the wound, liquefying and separating necrotic tissue from healthy tissue. |
| Sharp or surgical debridement. | This procedure removes the necrotic tissue and senescent cells that slow down the tissue repair process, converting a chronic wound into an acute one in the process. |
| Mechanical debridement. | It involves allowing a traditional gauze-type dressing to dry out and adhere to the surface of the wound before manually removing the dressing, debriding any tissue attached to it. |
| Electrical stimulation. | Stimulation of many cellular processes improves healing. |
| Biosurgery. | Therapeutic use of live blowfly larvae (maggots) for quick debridement. |
| Topical growth factors. | Nerve-growth factors, colony-stimulating factors, and fibroblast growth factors are found to be effective in treating diabetic and venous ulcers. |
| Negative pressure wound therapy. | A wound dressing system that continuously or intermittently apply a subatmospheric pressure to the surface of a wound to assist healing. |
| Enzymatic debridement (chlorophyll, collagenase, papain). | Enzymatic debridement uses proteolytic enzymes to remove necrotic tissue. These agents work by selectively digesting the collagen portion of the necrotic tissue. Care should be taken to prevent damage to surrounding healthy tissues. |
Nursing Care Plan Based on Risk for Infection Diagnosis – Nursing Care Plans for Pressure Ulcers
Nursing Diagnosis: Risk for Infection
Risk factors
Poor nutritional status.
The proximity of sacral wounds to the perineum.
Open pressure ulcer.
Desired Outcomes
- The client will maintain a normal body temperature.
- The client will remain free of local or systemic infections, as evidenced by the absence of copious, foul-smelling wound exudate.
| Nursing Interventions | Rationale |
| Assess the client’s nutritional status. | Clients who seriously lack nutrition (serum albumin <2.5 mg/dl) are at risk of developing infection produced by a pressure ulcer. Also, clients with pressure ulcers lose tremendous amounts of protein in wound exudate and may require 4000 kcal/day or more to remain anabolic. |
| Assess the client for unexplained sepsis. | When septic workup is done, the pressure ulcer must be considered a possible cause. |
| Assess for urinary and fecal incontinence. | Sacral wounds, because of their proximity to the perineum, are at the highest risk for infection caused by urine or fecal contamination. It is sometimes difficult to isolate the wound from the perineal area. |
| Assess pressure ulcers for odour, the colour of tissue, and drainage. | Foul-smelling pressure ulcer may indicate an infection; Infected tissue usually has a gray-yellow appearance without evidence of pink granulation tissue; The presence of exudate that is clear to straw-coloured is normal. While purulent green or yellow drainage in large amounts indicates an infection. |
| Assess the client’s temperature. | Fever is considered a temperature above 100.4 degrees F (38 degrees C) indicate a presence of infection unless the client is immunocompromised or diabetic. |
| Monitor the client’s white blood cell count (WBC). | Elevated WBC counts indicate an infection, although, in very old individuals, the WBC count may rise only slightly during infection, indicating a diminished marrow reserve. |
| Obtain wound cultures, if indicated. | All pressure ulcers are colonized because skin normally has flora that will be found in an open skin lesion; however, all pressure ulcers are not infected. Infection is present when there is copious, foul-smelling, purulent drainage and the client has other signs of infection (fever, increased pain) and bacteria count greater than 105. Swab cultures are not recommended. Rather, tissue biopsy should be used to quantify and qualify the aerobic and anaerobic organisms present. |
| Consult with a dietitian for assistance with a high-protein, high-calorie diet. | A High-calorie, high-protein diet may be recommended to help in healing and resist infection. |
| Provide thorough perineal hygiene after each episode of incontinence. | This can lessen pathogens in the area of sacral pressure ulcers. |
| Provide hydrotherapy, if indicated. | It is used to achieve wound cleansing and to promote good circulation. |
| Administer antibiotics as prescribed. | Complicated wounds may develop cellulitis or sepsis, requiring antibiotic therapy. Oral antibiotics or topical silver sulfadiazine can be effective. |
| Provide local wound care as prescribed. | The type and level of wound treatment depend on the staging of the ulcer and the type of infection present. |
As you continue, customnursingassignments.com has the top and most qualified writers to help with any of your assignments. All you need to do is place an order with us. (Nursing Care Plans for Pressure Ulcers)

Nursing Care Plan Based on Risk For Ineffective Health Maintenance Diagnosis – Nursing Care Plans for Pressure Ulcers
Nursing Diagnosis: Risk for Ineffective Health Maintenance
Risk factors
Impaired functional status.
Lack of previous similar experience.
Need for long-term pressure management.
Possible need for special equipment.
Desired Outcomes
Client and caregiver will verbalize understanding of the following aspects of home care: nutrition, pressure relief, wound care, and incontinence management.
Client and caregiver will verbalize ability to cope adequately with an existing situation, provide support/monitoring as indicated.
| Nursing Interventions | Rationale |
| Assess the client’s and caregiver’s knowledge of and ability to provide local wound care. | Client’s are no longer kept hospitalized until pressure ulcers have healed. The need for local wound care may continue at home for weeks to months. |
| Assess the client’s and caregiver’s understanding of the prevention of further pressure ulcer development. | Clients who are immobile will need frequent repositioning to lessen the risk fro breakdown in those areas that are intact. |
| Assess the client’s and caregiver’s understanding of the long-term nature of wound healing | Pressure ulcers may take weeks to months to heal, even under ideal circumstances. Wound heal from the base of the ulcer up and from the edges of the ulcer toward the center. Palliative wound care may be appropriate for a clean, chronic, non-healing wound. |
| Assess the client’s and caregiver’s understanding of the relationship between incontinence and further skin breakdown or complication of healing. | Managing incontinence may be the most difficult aspect of home management and is often the reason for nursing home placement are made. |
| Assess the client’s and caregiver’s understanding of and ability to provide a High-calorie, high-protein diet throughout the course of wound healing. | Clients may require enteral feeding (through gastronomy tube, nasogastric tube feedings, or the oral route), which requires knowledge of preparation and the use of special equipment. |
| Assess for the availability of a pressure reduction or pressure-relief surface. | A client may take a thick, dense foam mattress home from the hospital to place it on their own bed. Rental provisions of low-air-loss beds (e.g., KinAir, Flexicare) and air-fluidized therapy beds (FluidAir, Skytron, Clintron) may be arranged but often pose a financial difficulty because few payer sources will cover the cost of these beds in the home. |
| Educate the client and the caregiver to report the following signs indicating wound infection: Fever, malaise, chills, foul-smelling odour, purulent drainage. | Early detection prompts immediate intervention. |
| Educate the client and the caregiver in managing incontinence (e.g., use of moisture barrier ointments, use of underpads, use of external catheters). | Teaching proper techniques can prevent leakage and skin problems. Reusable products such as underpads or linen protectors made of cloth with a waterproof lining are better for the client’s skin and are more economical but require laundering. Moisture barrier ointments protect intact skin from excoriation. |
| Educate the client and the caregiver regarding local wound care, and allow for a return demonstration. | This will allow the client to use new information immediately, thus enhancing retention. Immediate feedback allows the learner to make corrections rather than practice the skill incorrectly. |
| Provide written instructions with listed resources. | Long-term management requires specific written plans to enhance adherence o treatment. Several internet resources provide lay education. |
| Involve a social worker or case manager. | Referral helps the client and family determine whether placement in an extended care facility is needed. Because many clients with pressures are older, it is often an older spouse who is available to provide care; as a result of the intensive nursing care needs of these clients, discharge to home is often unrealistic. |
| Consult a wound specialist to evaluate care in the home. | Besides evaluating the ability to deliver care, the specialist may be useful in securing specialty treatment. |
| Educate the client and the caregiver on the importance of pressure reduction and relief (e.g., turning schedule, use of specialty beds, use of relief surface where the client sits). | Information can nurture enhanced adherence to pressure ulcer treatment guidelines. |
| Discuss with the client and caregiver the possible need for respite care. | Long-term responsibility for client care in the home is burdening; those providing care may need help to understand that their needs for relaxation are important to the maintenance of health and should not be viewed as avoidance of the responsibility. |
| Discuss with the client and caregiver the need for in-home nursing care or homemaker services. | These provide all or part of the client’s care and can be economical to the client. Also, keeping the client in his or her own environment lessen the risk for hospital-acquired infection and keeps the client in familiar surrounding. |
Summary
Patients of all ages are susceptible to pressure ulcers, which are particularly common among diabetics. Prolonged bed rest (at least 8 hours at a time), starvation, dehydration, poor circulation, edema, and lack of mobility are the major causes. Pressure ulcer severity is divided into four stages: stage I, stage II, stage III and stage IV.
Proper wound care products, such as topical negative pressure dressings, support surfaces, padding, and bandages, are the greatest strategy to avoid ulcer formation. Giving patients well-balanced food, as well as keeping them hydrated and mobile, will aid in their recovery.
Related FAQs – Nursing Care Plans for Pressure Ulcers
1. What are the 4 stages of pressure ulcers?
These are:
- Stage 1. The area looks red and feels warm to the touch. …
- Stage 2. The area looks more damaged and may have an open sore, scrape, or blister. …
- Stage 3. The area has a crater-like appearance due to damage below the skin’s surface.
- Stage 4. The area is severely damaged and a large wound is present.
2. What is the best treatment of pressure ulcers?
Clean open sores with water or a saltwater (saline) solution each time the dressing is changed. Putting on a bandage. A bandage speeds healing by keeping the wound moist. It also creates a barrier against infection and keeps skin around it dry.
3. What are the common symptoms of a pressure ulcer?
Warning Signs and Symptoms of Pressure Ulcers
- A change in the colour of the skin. …
- Reddening of the skin that does NOT turn white when you press it. …
- Any unusual changes in skin texture may be related to pressure damage. …
- A patch of skin that feels cooler or warmer to the touch than others.
- A sore or itchy patch of skin.
4. What antibiotics are used for pressure ulcers?
Amoxicillin-potassium clavulanate is a naturally occurring beta-lactam structurally similar to the penicillin nucleus. This antibiotic group of beta-lactam/beta-lactamase combination has demonstrated a broad-spectrum activity; therefore, it is frequently used for the treatment of infected pressure ulcers.
